Who performs varicose vein surgery?
The following specialists perform surgery on varicose veins:
- General Surgeons
- Vein Specialists
- Vascular surgeons
- Phlebologists
- Dermatologists
Why is vein surgery performed on varicose veins?
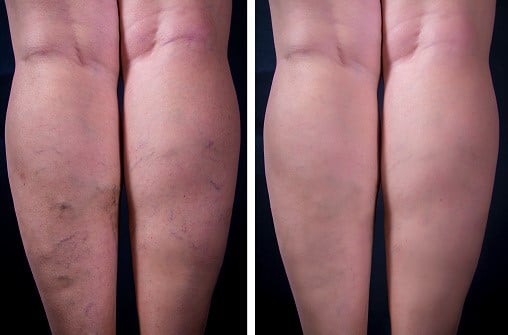
Varicose veins that are large, protruding out, or unsightly. Surgery may also be appropriate if your varicose veins are causing symptoms such as burning, aching, soreness, and cramping.
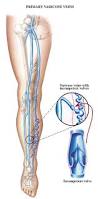
Veins are blood vessels that carry blood from your body back to the heart. Valves inside the veins help direct blood back to the heart. When valves are damaged or weakened, blood can pool up in the veins which causes them to swell and weaken. Varicose veins occur as a result of this.
Your healthcare provider may consider varicose vein surgery for you only if other treatments have been ineffective. Ask your doctor about other options of less invasive treatment to find the best treatment for your situation.
How is this surgery performed?
Varicose vein surgery is performed in doctor’s offices, surgical centers, and hospitals depending on your given situation. One or more types of anesthesia will be used including:
- General anesthesia is administered via IV and gases are given to put the patient into a deep sleep.
- Local anesthesia is administered via injection around certain nerves to numb the area desired.
What to expect the day of your surgery?
Varicose vein surgery that only use local anesthesia includes the following steps:
- Change into a patient gown
- Your doctor will mark the veins with a pen to identify them
- You will lie on the exam table to allow access to the surgeon
- Your doctor/surgeon will prepare the skin by cleaning the area
- The local anesthetic will be injected and you will remain awake during the procedure
Why the AVC doesn’t use General Anesthesia for Vein Surgery
Varicose vein surgery that uses general anesthesia includes the following steps:
- Talk with your pre-operative nurse who will perform an exam and check to ensure all needed tasks are completed and the consent form is signed
- The surgical team will instruct you to change into a patient gown
- Talk to your anesthesiologist or nurse about your medical history and the type of anesthesia you will be receiving
- A surgical team member will administer an IV
- The anesthesia will be started
- For general anesthesia, your anesthesiologist or nurse will place a tube into your lungs to protect and control breathing safely. You will not remember this or the procedure
- Your doctor will use small incisions, surgical techniques, and instruments to close off or remove the varicose veins
- The surgical team will monitor your vital signs throughout the procedure and while recovering to ensure safety
Often referred to as ambulatory phlebectomy, this is a minimally invasive alternative to older vein stripping procedures discussed earlier. During microphlebectomy, the insufficient vein is removed via the leg through small punctures in the skin. This is often combined with EVLA, and has a high rate of effectiveness because it completely removes the varicose vein. It is performed under local anesthesia and does not require stitches or sutures.
Can vein surgery be used to treat varicose veins and spider veins?
Yes, vein surgery can be used to treat both varicose veins and spider veins, although the specific type of surgery may vary depending on the condition being treated.
For varicose veins, which are larger, bulging veins usually found in the legs, vein surgery may involve procedures such as vein ligation and vein stripping, or more minimally invasive techniques like endovenous laser treatment (EVLT) or radiofrequency ablation (RFA).
Is vein surgery covered by insurance?
Whether vein surgery is covered by insurance depends on several factors, including the type of surgery, the reason for the surgery, and your insurance policy. In general, vein surgery may be covered by insurance if it is deemed medically necessary to treat a specific condition that is causing symptoms or complications.
Can vein surgery be performed on people with certain medical conditions, such as diabetes or heart disease?
Vein surgery can be performed on people with certain medical conditions, but it depends on the specific condition and its severity. For example:
1. Diabetes: People with diabetes may undergo vein surgery, but they require careful monitoring and management of their blood sugar levels before and after surgery to reduce the risk of complications such as infection and delayed wound healing.
2. Heart disease: People with heart disease may undergo vein surgery, but their heart condition will be carefully evaluated to ensure that they can tolerate the surgery and anesthesia. Precautions may be taken to reduce the risk of complications during and after surgery.
What Are Signs Of Blood Clot After A Vein Surgery?
If you suspect you might have a blood clot after a vein surgery, then you should look for signs like persistent swelling in the leg, redness, warmth, and tenderness along the veins. Usually after the surgery, your pain and discomfort is supposed to get better, but in this case it will get worse, especially in the calf it may even indicate deep vein thrombosis (DVT). In some rare cases, it’s possible for the clot to even travel to the lungs ans cause problems like shortness of breath, chest pain, dizziness, or rapid heartbeat, which is a case of an emergency! Experiencing any of these symptoms can be quite scary, if you do then make sure to inform your doctor and seek medical attention as soon as possible. Doctors can provide with the treatments like compression stockings, to help you deal with swellings and formation of blood clots, or blood thinner to avoid blood clots at all costs.
Is Vein Surgery Safe For Elderly People?
Yes, fortunately even for older people vein surgery is quite safe and effective, but it depends mostly on your overall health and medical history, since there are some health conditions that might make it harder for you to get the treatment or might later cause side effects. If older adults suffer from problems like heart disease, diabetes, or poor blood circulation then it might not be the best treatment for them as they are known to impair with healing and increase the risks of complications like infection. Which is why, for older patients minimally invasive are used much more often, these can include treatments like sclerotherapy or laser treatments. They have much shorter recovery time and do not cause any serious complications as well, make them just the best options for elderly people. However, this doesn’t mean, older people can’t get be in surgery, they just need to make sure they have a good overall health.
Can I shower or bathe after vein surgery?
After vein surgery, your healthcare provider will provide specific instructions regarding bathing and showering. In general, you may be advised to wait a certain amount of time before showering or bathing to allow your incisions to heal properly.
What to expect after varicose vein surgery?
You will remain in the recovery room until you are alert and your vital signs remain consistent. A sore throat may be common due to the tube used during surgery. It is common that patients walk and go home the same day as surgery if all recovery procedures are met. One day of hospital stay may be needed in other cases. Compression stockings may be needed to stabilize the veins and promote the healing process.
Recovery time following surgery is a process that varies in length. This is dependent upon the procedure type, type of anesthesia, your health, age, etc. It may be days or even weeks to achieve a full recovery.
Pain management is very important to the recovery process. Discomfort will most likely be present following surgery. Your doctor will treat your pain to provide comfort and the ability to rest. Inform your doctor if your pin levels increase or change in any way.
Keeping follow-up appointments following surgery for varicose veins is important.
Contact your doctor right away or seek medical attention if you are experiencing the following:
- Breathing problems, such as shortness of breath, difficulty breathing, labored breathing, or wheezing
- Change in alertness such as passing out, dizziness, unresponsiveness, or confusion
- Fever. A low-grade fever (lower than 101 degrees) is common for a couple of days after surgery and not necessarily a sign of a surgical infection.
- Leg pain, redness or swelling, especially in the calf region, which may indicate a blood clot
- Pain that is not controlled by your medication
- Unexpected drainage or pus coming out of an incision
How will this surgery affect my day to day life?
Varicose vein surgery has the potential to cure your condition or greatly reduce your symptoms. Much of the bulging, discomfort, and discoloration from varicose veins will achieve relief. The surgery will not prevent varicose veins from coming back, and more surgery may be needed in the future.
Changes in your lifestyle that may help prevent or delay the recurrence of varicose veins include the following:
- Exercise regularly
- Losing weight
- Wear compression stockings
Minimally Invasive Varicose Vein Treatment Options
Varicose vein treatment in the past has been known to be limited in the number of treatment options. It used to only be known for a painful and invasive procedure known as vein stripping, where the insufficient vein is surgically removed. This procedure requires general anesthesia, an overnight stay, and a lengthy time period of recovery. Today, varicose vein treatment has graduated to more procedures that are minimally invasive and less painful. These new methods of treatment are more effective at treating venous insufficiency.
The Advanced Vein Center offers endovenous Radiofrequency ablation -RF, much like (EVLA), sclerotherapy, and microphlebectomy to patients who are interested in minimally invasive vein procedures. The procedures vary in how the symptoms are treated based on the individual. An in-person consultation and ultrasound diagnosis will be done by the doctor. In most cases, multiple procedures are prescribed for optimal results.
RF like Endovenous Laser Ablation (EVLA)
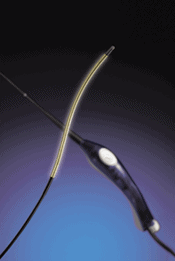
This is also known as endovenous RF treatment, Closure Fast Cath implements the use of laser like Microwave tips to heat and seal insufficient veins. This procedure is minimally invasive, and is done by the placement of a thin fiber catheter into the desired vein through a 1mm area. After insertion, the tip is slowly drawn back through the vein while it emits thermal energy to the surrounding walls of veins. Performed under local anesthesia, this procedure causes little to no discomfort and has minimal side effects or recovery time.
Sclerotherapy
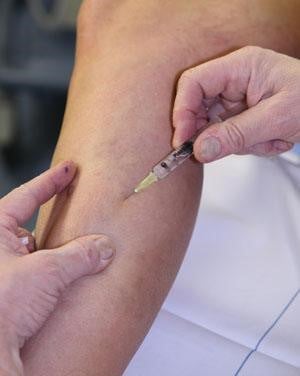
This commonly used injectable vein treatment is commonly used for eliminating spider and varicose veins. First, a chemical agent known as sclerosant is injected into the problem vein. This causes the vein to become irritated and inflamed, which prompts it to seal and remove itself from circulation. This is usually the choice to treat smaller insufficient veins because the body will safely and naturally absorb the treated vein. Minimal side effects and downtime are expected for most cases.
Microphlebectomy