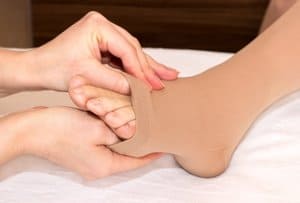
At the Advanced Vein Center, we believe in treating the source of vein problems, not just the symptoms! Compression Therapy is the first step!
Many skin care centers that treat aesthetically displeasing leg veins focus on injecting the legs with sclerotherapy. However, patients with serious leg swelling and discoloration from long standing vein disease need true medical vein treatment. Serious treatment of vein disease begins and ends with the compression therapy and management of leg edema.
Before starting any vein intervention, it is important to have an accurate assessment of the problem.
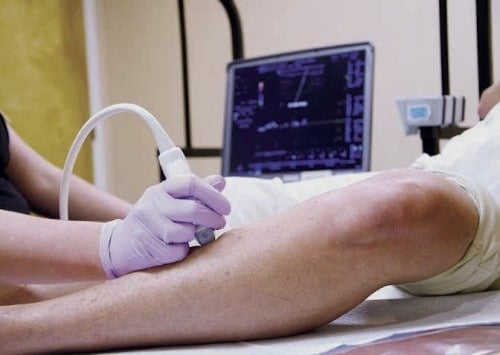
The best vein evaluation includes:
- A Doppler Ultrasound to diagnose vein disease.
- A full Medical History and Physical Assessment.
- Confirmation of what treatments insurance covers as some patients will choose not to have compression garments if they are not covered by insurance.
Insurance for Compression Therapy
Many Insurance companies require a course of compression therapy for swollen legs before they will consider paying for vein surgery or any other vein procedures. Although compression won’t change the underlying vein disease, it may help control painful and destructive vein symptoms while you wear them.

Not all stockings are created equal! Compression vein stockings have a compression gradient. This gradient means they are stronger at the bottom than at the top. Because gravity causes more blood pooling and swelling farther away from the heart and lower to the ground, it’s important for them to work more where they are needed the most.
Compression garments come in different materials, colors, and textures:
- Cotton sport sock styles for men and athletes
- Black dress sock styles for use with trousers
- Varieties of colors and patterns
- Standard tan/beige
- Open toe and closed toe options.
Why should I wear compression stockings?
Compression Therapy for Poor Circulation

Compression stockings are worn to assist with circulation, provide support to the legs and veins, and diminish swelling. The compression is graduated, with the strongest support starting at the ankles and gradually decreasing towards the top of the garment. As a person moves, graduated compression stockings apply pressure to the outside of the veins to help reduce their size, help the valves close and aid in returning blood back to the heart. The combination of graduated compression stockings plus leg activity can help improve blood circulation and give you more freedom to move.
Poor Circulation can lead to skin ulcers. When veins become weak, enlarged or overstretched and valves don’t work properly, this allows poor circulation to occur in your lower leg, possibly resulting in chronic venous insufficiency and a breakdown of skin known as leg ulcers.
Chronic venous insufficiency can result in several complications, including swollen achy legs, pain, deep vein thrombosis, spider and varicose veins, and venous leg ulcers. Ulcers or wounds usually occurs above the ankle and below the calf and refuses to heal or heals slowly.
Compression therapy address circulation problems by supporting the leg muscles and veins. This support increases circulation in your leg. Maintaining good circulation is crucial to preventing and managing these types of open wounds and decreasing the risk of recurrence.
Compression Therapy for Lymphedema
Lymphedema is a condition that affects the lymphatic vessels, which are responsible for transporting protein-rich lymph fluid back into the circulatory system. When lymph vessels are unable to transport this fluid properly, a build-up occurs, resulting in swelling and thickening of the skin. This usually occurs on an arm or a leg. Lymphedema can be either primary or secondary. This means it can occur on its own (primary lymphedema), or it can be caused by another disease or condition (secondary lymphedema). Secondary lymphedema is more common than primary lymphedema.
Although there is no cure, wearing compression garments is one of the most important aspects of managing lymphedema. Compression garments are designed to keep a continuous pressure on the swollen areas to assist the drainage of fluid and minimize swelling.
Treatments for Lymphedema
There’s no cure for lymphedema.
Treatment focuses on reducing the swelling and controlling the pain.
Lymphedema treatments include:
Exercise – Light exercises in which you move your affected limb may encourage lymph fluid drainage and help prepare you for everyday tasks, such as carrying groceries. Exercises shouldn’t be strenuous or tire you but should focus on gentle contraction of the muscles in your arm or leg. A certified lymphedema therapist can teach you exercises that may help.
Wrapping your arm or leg – Bandaging your entire limb encourages lymph fluid to flow back towards the trunk of your body. The bandage should be tightest around your fingers or toes and loosen as it moves up your arm or leg. A lymphedema therapist can show you how to wrap your limb.
Massage – A special massage technique called manual lymph drainage (MLD) may encourage the flow of lymph fluid out of your arm or leg. Various massage treatments may benefit people with active cancer. Be sure to work with someone specially trained in these techniques. Massage isn’t for everyone. Avoid massage if you have a skin infection, blood clots or active disease in the involved lymph drainage areas.
Pneumatic Compression – A sleeve worn over your affected arm or leg connects to a pump that intermittently inflates the sleeve, putting pressure on your limb and moving lymph fluid away from your fingers or toes.
Compression Therapy – Long sleeves or stockings made to compress your arm or leg encourage the flow of the lymph fluid out of your affected limb. Wear a compression garment when exercising the affected limb. Obtain a correct fit for your compression garment by getting professional help. Ask your doctor where you can buy compression garments in your community. Some people will require custom-made compression garments. If you have difficulties putting on or taking off the compression garment, there are special techniques and aids to help with this; your lymphedema therapist can review options with you. In addition, if compression garments or compression wraps or both are not an option, sometimes a compression device with fabric fasteners can work for you.
Can facial fat transfer be used to treat specific facial concerns, such as sunken cheeks or hollow under eyes?
Yes, facial fat transfer can be used to treat specific facial concerns such as sunken cheeks or hollow under eyes. By injecting fat into areas of the face that have lost volume or appear sunken, facial fat transfer can help restore a more youthful and rejuvenated appearance. This procedure is particularly effective for filling in hollow areas and adding volume to areas that have lost fat due to aging or other factors. The fat used in the transfer is typically harvested from another area of the body, such as the abdomen or thighs, and then purified before being injected into the desired areas of the face.
What factors can affect the success of facial fat transfer?
Several factors can affect the success of facial fat transfer, including:
- Harvesting Technique: The technique used to harvest the fat can impact the viability of the fat cells. Gentle harvesting and processing techniques are crucial to ensuring the survival of the transferred fat cells.
- Purification Process: The fat must be purified before it is injected into the face to remove impurities and excess fluids. Proper purification helps increase the longevity of the transferred fat cells.
- Injection Technique: The skill and experience of the surgeon performing the fat transfer procedure can significantly impact the success of the treatment. Precise injection techniques are necessary to achieve natural-looking results and ensure the fat cells survive.
- Patient’s Health: The overall health and lifestyle habits of the patient can affect the success of facial fat transfer. Factors such as smoking, alcohol consumption, and certain medications can impact the healing process and the survival of the transferred fat cells.
- Postoperative Care: Following postoperative care instructions, such as avoiding strenuous activities and wearing compression garments, is crucial for the success of facial fat transfer.
Compression Therapy FAQ
Elevation, elevation, elevation!
Leg swelling occurs when the valves in the leg veins fail and gravity pools the blood down to your feet and ankles. Have gravity work for you rather than against you and “put your feet up” whenever you get a chance!
Arteries have muscle tissue in their walls, veins do not.
You rely on your calf muscles surrounding the veins in your legs to pump the blood against gravity, back to the heart.
The stronger your leg muscles are from walking and exercise, the more strongly they can pump the blood in the veins.
Besides swollen legs, which is called edema, major symptoms of vein disease include brownish discoloration around the ankles and breakdown of the skin. Minor vein disease symptoms are itchiness which increases as the day goes on, night cramps and restless leg symptoms.
Exposure to sun is very damaging to veins. The sun and heat cause the elastic to release and makes swelling worse, leading to blood leaking out of the vein. The hemoglobin from the escaped blood stains and discolors the skin. This then goes on to weaken the skin and can lead to leg ulcers.
Saunas, Jacuzzis and Hot Tubs also cause increased stress on the veins.
After a vein procedure you NEED to WEAR COMPRESSION GARMENTS!
How long you need to wear your stockings and the best type to get is up to your vein specialist.
Drink several glasses of water daily. Never take Ibuprofen, Aleve or other NSAIDS and especially no Aspirin for several days. Take only Tylenol for discomfort, as the other medications can thin your blood and increase bleeding complications.
Cold packs are a simple, safe alternative to pain medicine to sooth local pain and inflammation after a vein procedure. A small amount of discomfort is normal; but, if you experience severe pain or bleeding, call your vein surgeon immediately and go to an emergency room if bleeding is out of control.
