RF Vein Treatment
The RF procedure, or “RF” for short, was approved by the United States Food and Drug Administration (FDA) in 1999. It’s undergone several refinements since then and is now the standard RF vein treatment for lower extremity vein disease (venous reflux). At present the procedure can be done in-office by most general surgeons, vascular surgeons, and phlebologists. The Venefit system by Covidien Medical is arguably the most widely used RF closure technique in use today.
As mentioned, the process itself typically lasts less than one hour. To start, the patient is gowned and the leg being treated is sterilized. Then a Registered Vascular Technologist (RVT), aka ultrasound tech, assists the surgeon in finding the location of the diseased vein.
Nerve Protection
Since RF Vein Treatment is heat-based it has the potential to damage surrounding tissue. To work around this problem, as well as to provide pain control, large amounts of highly diluted anesthetic fluid into the space surrounding the vein. For many surgeons, lidocaine is the anesthetic of choice. This is accomplished using a standard surgical pump. Not only does this fluid barrier protect the surrounding tissue but it provides pain control as well. Patients typically feel a pressure sensation but never outright pain or discomfort.
RF Procedure
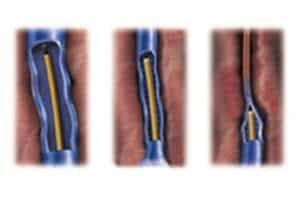
Next, the surgeon makes a tiny incision to access the vein. This is usually done at or near the ankle in order to treat the entire length of the diseased vein. With the RVT’s help, the surgeon inserts a specialized catheter up the length of this vein. What makes this piece of disposable medical device unique is its tip, which contains a heating element.
Note that only at this point does the actual RF Vein Treatment begin—everything up to this point has been preparation. Radiofrequency (RF) energy is then delivered through this catheter to the element to produce heat. This delivers very high temperature spikes for very short periods of time. This damages the vein enough to cause the formation of scar tissue. As the catheter is withdrawn each segment is treated, one at a time, along the course of the vein. This treatment phase takes under 5 minutes.
As the vein scars down it collapses. Finally, in the months following the procedure it is broken down by the body. Eventually the vein is reabsorbed entirely.
Benefits Of RFA
1. Quick and secure
The typical time for an outpatient RFA procedure is 35 to 40 minutes. The procedure’s non-surgical nature eliminates the hazards associated with surgery.
2. minimally harmful
RFA may treat an entire vein up to 30 inches in length with just a short, 14 inch incision.
3. Almost no pain
You shouldn’t feel anything because the doctor will administer local anaesthetic to the area before doing the RFA technique. If you have any pain or discomfort thereafter, it will be minimal.
4. The effects might be long-lasting.
The possibility of permanent results is yet another advantage of this therapy. The unhealthy veins are removed, as is the case with the majority of conventional varicose and spider vein treatments. With this procedure, the walls of the veins that are being treated collapse in on themselves. The targeted veins are effectively eliminated when the venous walls give way. Yet it takes a few weeks for the veins to stop receiving blood and disappear.
The most crucial thing to comprehend is that sickness rarely causes healthy veins to become gnarled and twisted.
Consequently, you could only only one treatment session to achieve your ideal outcomes, depending on the number of varicose or spider veins you need to treat, their size, the reason they are disordered, and where they are located.
5. It Is Without Needles
The most common non-invasive varicose and spider vein treatment is sclerotherapy, however it is not appropriate for everyone. Sclerotherapy’s main drawback is that treatment necessitates the injection of a saline solution. Sadly, many people dislike the concept of being injected, even with merely seawater, or are scared of needles.
Am I eligible for RFA?
The best approach to find out if you qualify is to get a consultation and thorough evaluation from a qualified pain specialist.
Your doctor conducts a physical examination in addition to reviewing your medical history and talking about your present symptoms. Also, our team runs any essential testing to rule out any underlying diseases that would make RFA an ineffective treatment option.
RFA is typically an useful alternative for people whose pain has subsided following a brief diagnostic nerve receptor block. RFA is not a smart choice, however, for pregnant women or those who may get pregnant, persons with bleeding issues, or those who are currently ill.
Can RF vein treatment be used on pregnant women?
RF vein treatment is generally not recommended for pregnant women. During pregnancy, hormonal changes and increased blood volume can lead to the development or worsening of varicose veins and other vein issues. However, treating these vein conditions with procedures like RF vein treatment is typically deferred until after pregnancy due to the potential risks to the developing fetus.
Is there any downtime after RF vein treatment?
The downtime after RF vein treatment is typically minimal. Most people are able to resume their normal activities immediately after the procedure. However, it’s common to experience some mild discomfort, bruising, or swelling at the treatment site, which may limit certain activities for a short period of time.
Who is a good candidate for RF vein treatment?
A good candidate for RF vein treatment is someone who has varicose veins or other venous insufficiency issues and has not responded well to conservative treatments such as compression stockings or lifestyle modifications. Ideal candidates typically have:
1. Varicose veins that are causing symptoms such as pain, swelling, or discomfort.
2. Visible varicose veins that are cosmetically bothersome.
3. Failed previous treatments for varicose veins.
4. No significant medical conditions that would make the procedure risky.
5. Realistic expectations about the outcome of the procedure.
What should I do to prepare for an RF vein treatment procedure?
To prepare for an RF vein treatment procedure, you may be advised to take the following steps:
1. Inform your healthcare provider about any medications you are taking, including over-the-counter and prescription medications, as well as any supplements.
2. Follow any pre-procedure instructions provided by your healthcare provider, such as fasting before the procedure if required.
3. Arrange for someone to drive you home after the procedure, as you may be advised not to drive immediately afterward.
4. Wear loose, comfortable clothing on the day of the procedure
How Does RF vein Treatment Compared To Laser Vein Treatment?
Both radiofrequency vein treatment an laser treatment are great options for treating minimally invasive procedures in minimally invasive ways, but both treatments use different methods and comfort. For example, RF treatment uses heat from radiofrequency energy to close off the vein, while laser treatment focuses on using laser energy to destroy the troubled veins. In general, radiofrequency treatment is considered less painful and causes really less bruises compared to the laser treatment, which in return also makes the recovery much faster. But when it comes to effectiveness, laser treatment is much more effective for smaller veins. However, despite few draw backs, in the end both treatments have high success rates. But RF is much more likely to be picked because it’s much more comfortable. Though the choices also depend on, locations of the veins, vein size and individual medical consideration.
How many sessions are typically required for RF vein treatment?
The number of RF vein treatment sessions needed varies based on the severity and size of the veins being treated. For larger varicose veins, most patients require only one session per affected vein, as the procedure effectively closes the vein in a single treatment. However, for extensive vein issues or multiple veins, additional sessions may be necessary. Follow-up appointments are usually scheduled to monitor healing and determine if further treatment is needed. Smaller veins or residual varicosities might require secondary treatments, such as sclerotherapy. Most patients experience significant improvement within a few weeks to months after the initial session.
Is RF vein treatment safe?
Yes, RF vein treatment is considered a safe and effective procedure for treating varicose veins. It is a minimally invasive technique approved by medical authorities and widely used by vascular specialists. The procedure involves inserting a catheter into the affected vein and using radiofrequency energy to seal it shut. While generally safe, some minor risks include bruising, swelling, mild pain, or temporary numbness.