Glue Vein Treatment, Pittsburgh
About VenaSeal Closure System
The VenaSeal Closure System is the most modern non-surgical procedure used to safely and effectively treat varicose veins.
The VenaSeal™ system uses a medical adhesive to close superficial veins in adults with symptomatic venous reflux of truncal like the Greater Saphenous Vein (GSV) permanently. It is different from other treatments in that it does not require multiple injections of large amounts of tumescent anesthesia around the vein. Instead, there is typically only one injection of local anesthesia.
The VenaSeal™ Closure System also removes the need for thermal energy to permanently close the veins. This means that the risk of nerve or skin damage is reduced. Healing time is also reduced since the medical adhesive sets within minutes.
Recovery time is significantly decreased with the VenaSeal™ Closure System. There is no longer a need to wear compression stockings after the procedure, and many patients return to work and normal activity right away. The entire procedure can be performed in just 20 minutes without the need for a general anesthetic.
BENEFITS OF VENASEAL CLOSURE SYSTEM
- No general anesthetic required
- Most people report only mild discomfort during the procedure
- The procedure can be performed within 30 minutes -no need to miss a whole day of work!
- Recovery time is minimal, most people can return to work and resume normal activities right away.
WHAT TO EXPECT
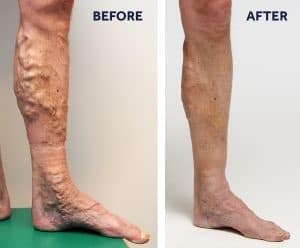
Your doctor will discuss your goals for the procedure with you and determine the best course of treatment. This is done after a Doppler Ultrasound is used to diagnose venous reflux and map your vein anatomy. If you have reflux (leaking vein valves), that are symptomatic- itching, cramping, aching, swollen- then you are a candidate. Unlike other treatments for varicose veins, there are no steps or preparations that you need to take at home before being treated with the VenaSeal Closure System. As with any procedure and to allow the “glue” to set properly, we do recommend that someone be there to drive you home.
During
The procedure can be performed in 20 minutes – no need to miss a whole day of work! Most people report only mild discomfort during the procedure. The procedure is performed using ultrasound to precisely guide the application of “glue” into the vein. See our video…

After treatment, most people are able to return to work and resume normal activities right away. There is little to no bruising and no need for compression stockings, although some patients may see a benefit from wearing them. In rare cases follow-up treatment may be required. The body naturally absorbs the small amount of glue used to seal off the vein.
Varicose Veins and the VenaSeal System.
The US Food and Drug Administration (FDA) has recently approved the VenaSeal
Closure system by Covidien LLC. It’s currently being used as a minimally invasive and permanent treatment for varicose veins.
Varicose Veins Are Extremely Common.
They’re can be quite unsightly as well. What’s worse, they often come along with symptoms such as achiness, swelling, and an uncomfortable tired, heavy feeling. At any given time, varicose veins affect about 25 million Americans.
The VenaSeal system by Covidien is unlike other modern varicose vein VenaSeal simply seals them shut. This immediately alleviates symptoms and improves appearance. It’s nearly 100% effective, and boasts shorter recovery times than other minimally invasive procedures. It’s also just as permanent and safe as other competing techniques.
VenaSeal relies on the same surgical adhesive surgeons use to seal shut veins and arteries in the brain. It’s completely inert, and can’t break loose and lodge elsewhere in the body. “There’s essentially no risk,” says vascular surgeon Dr. William Maisel, director of the FDA’s Center for Devices and Radiological Health. “We’ve approved this system based on impressive safety data. It’s not our official stance, but if it’s safe enough to be used in brain surgery it’s safe enough to be used anywhere.”
Continues Maisel, “this adhesive approach doesn’t rely on heat so there’s no damage to surrounding tissue. Surgeons in the field are finding that there’s very little recovery time or downtime with this technique. There usually isn’t even bruising.”
FREQUENTLY ASKED QUESTIONS
Q: What is Tumescent Anesthesia?
A: Tumescent anesthesia is a local anesthetic that is used in other procedures used to treat varicose veins. It is injected around the vein being treated and requires multiple injection sites. Since the VenaSeal Closure System uses painless “glue” to treat the vein, it does not require the use of tumescent anesthesia. Instead, only one injection of local anesthesia is typically needed.
A: Most patients report little to no pain during the procedure.
Q: How much time will I have to take off work?
A: None! The VenaSeal™ Closure System was designed to make the recovery process as quick and easy as possible. Patients can resume activities immediately.
Q: How soon will I see results?
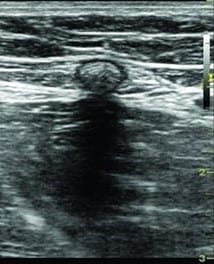
A: Results are immediate. Within 12 months after the procedure the vein turns into fibrous connective tissue that occludes the vein permanently, as seen on this ultrasound image
Important Safety Information – Risks, Warnings, Contraindications, Precautions and Complications of VenaSeal™
Closure System
- Use VenaSeal Closure System as a complete system, never use components separately.
- Should only be performed by endovenous trained Physicians
- For use in Superficial truncal veins only (GSV)
- Must have Ultrasound Guidance
CONTRAINDICATIONS:
- Sepsis (blood infection)
- Superficial Venous Thrombophlebitis
- Allergy or sensitivity to cyanoacrylates or VenaSeal adhesive
- Pregnancy
POTENTIAL ADDITIONAL RISKS AND COMPLICATIONS ( PLUS THOSE SIMILAR TO TRADITIONAL THERAPY)
Below is a list of the potential adverse effects (e.g., complications) associated with the use of the VenaSeal system. The adverse events associated with the device are similar to those with traditional endovenous thermal ablation procedures. In addition, there are several risks unique to the VenaSeal system due to its material and product design as an implant. These potential adverse events include, but are not limited to, the following:
- Leg swelling, hyperpigmentation, visible scars
- Blood clots in deep veins, Blood clot to lungs
- Bleeding and infection at catheter insertion site
- Superficial thrombophlebitis
- Bruising, collection of blood outside the vein
- Local numbness, pain, inflammation of vein and surrounding area
- Ulceration and itching at injection site
- Rupture or perforation of vein being treated
- A-V fistula
- Allergy to glue – hives, itching, anaphylactic shock
Traditional Treatments
There are several current treatments used in the medical community to treat chronic venous insufficiency. I will present you with the basics of the traditional treatments and many of their drawbacks below.
Conservitive treatments attempt to correct or improve the condition without surgery. They include:
- Compression Stockings,
- Exercise,
- Leg Elevation and
- Unna Boots
This modalities have the potential to slowly improve minor symptoms and have very few side effects.
Surgical procedures are more aggressive, showing more immediate results.
Surgical stripping is a common procedure where the great saphenous vein (GSV) is split at its confluence with the common femoral vein. The term stripping refers to the removal of a long vein segment. This modality has been in use for over 100 years. It is typically conducted in the operating room and requires general anaesthesia. It often requires up to 4 weeks of recovery time. There is a long incision scar that can lead to discomfort and will require wound care. After treatment, you will need to wear a compression stocking.
Thermal therapies apply heat (or other energy forms) to the veins. They can lead to:
- compression stockings,
- endothermal heat-induced,
- hematoma,
- hyperpigmentation,
- nerve injury,
- scarring,
- thrombophlebitis and
- thrombus (EHIT)
Opportunities for Advancement
Both surgical approaches and thermal therapies leave room for improvements. Many physicians have started turning to cyanoacrylate to aid in the process. Cyanoacrylate is a group of powerful, fast-acting adhesives with many medical applications. Those that have used cyanoacrylate have found that they eliminate:
- post-procedure pain and bruising,
- the need for post-procedure compression stockings and
- tumescent anesthesia
Cyanoacrylate Adhesives and Safety
Cyanoacrylate is FDA approved and is widely used as a medical tissue adhesive. It has an antimicrobial effect against gram-positive organisms. These bacteria include:
- anthrax (Bacillus anthracis),
- diphtheria (Cornynebacterium diphtheriae),
- pneumococci,
- staphylococci (“staph”) and
- streptococci (“strep”).
It has been used safely on millions of patients and according to a 1986 study, there is no danger of carcinogenicity in humans.
Why is cyanoacrylate ideal for venous closure?
Cyanoacrylate is used in a variety of medical procedures as a hemostatic agent or to “glue” tissues together in a surgical wound. it is widely used in orthopedic procedures to affix hardware. Additionally it has been used in plastic surgery for blood vessel anastomoses, wound closure, application of skin grafts, or hemostasis. Surgeons have found that cyanoacrylate has many advantages including:
- binding properties are not affected by moisture or blood,
- easy to use in the operating room,
- eliminates the need for compression stockings,
- encapsulated by the body just like a foreign body,
- ideal viscosity,
- polymerization starts when it comes into contact with blood or plasma,
- quick polymerize,
- retains strong adhesion,
- soft and elastic bond
- stimulates an inflammation in the vessel wall causing occlusion.
Is it any wonder that professionals who are looking to improve their patients’ experiences are starting to use cyanoacrylate?
Treating varicose veins safely with medical adhesive “superglue”
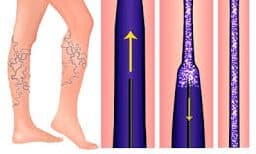
The VenaSeal vein glue system
For greater than 15 years, varicose veins have been successfully treated using two minimally invasive techniques. The first and most widely used is radiofrequency ablation (RF). The second is endovenous laser therapy (EVLT). Although both RF and EVLT treatments are effective and well-tolerated medical researchers are continually seeking less invasive options.
The most recent development involves the use of the medical-grade adhesive known as cyanoacrylate. Previously, this type of adhesive has been used to permanently seal cranial arteriovenous (AV) fistulas. Today it’s being used to permanently seal incompetent veins and varicose veins of the lower extremity. Clinically speaking this often refers to the great saphenous vein (GSV), small saphenous vein (SSV), or both.
During treatment cyanoacrylate adhesive is introduced directly into the vein being treated. The glue begins to permanently bond with the vein wall where it undergoes a hardening process (sclerosis). Once fully hardened the incompetent vein is sealed shut along its entire length and gradually reabsorbed by the body. The final effect is identical to that produced by the RF and EVLT techniques.
Among vascular specialist the VenaSeal brand cyanoacrylate adhesive is usually referred to simply as “vein glue.” To date the VenaSeal system is arguably the least invasive treatment in use today.
How is VenaSeal adhesive used?
During treatment, a specialized catheter is used to place a small amount of adhesive inside the vein being treated. This immediately removes the vein from the venous circulation. Due to the nature of the venous system the blood is immediately diverted into nearby healthy veins.
Technically speaking, treatment with VenaSeal is simpler and easier than either RF or EVLT. Pain control using local anesthetics isn’t required, nor is the introduction of large volumes of dilute anesthetic (tumescent anesthesia). No medications must be taken to prepare the patient for the procedure. Upon completion the patient can return to their full range of activities immediately.
Furthermore, since VenaSeal isn’t a heat-based treatment it carries no risk of burn injuries or nerve damage. This also means that no prescription pain medication is necessary after the procedure. Finally, the use of hot, uncomfortable compression stockings in the days following the procedure isn’t necessary.
How does vein glue treatment compare to traditional vein closure methods like vein stripping?
Vein glue treatment, also known as endovenous adhesive closure, offers several advantages over traditional vein closure methods like vein stripping. Unlike vein stripping, which involves the physical removal of the affected vein, vein glue treatment is minimally invasive. It uses a medical adhesive to seal the problematic vein shut, causing it to collapse and gradually disappear. Vein glue treatment typically requires smaller incisions, results in minimal scarring, and often involves less pain and a quicker recovery. Patients can usually resume normal activities sooner. Additionally, vein glue treatment can be performed on an outpatient basis, reducing the need for hospitalization, making it a preferred choice for many individuals seeking vein closure therapy.
Can vein glue be used in combination with other vein treatments?
Yes, vein glue treatment can be used in combination with other vein treatments, depending on the specific needs and conditions of the patient. This approach is often referred to as a “combination therapy” or “combined treatment plan.”
For example, vein glue treatment may be used in conjunction with procedures like endovenous laser therapy (EVLT) or radiofrequency ablation (RFA) to address different aspects of vein issues. In some cases, a patient may have multiple veins with varying degrees of severity, and a combination of treatments may be recommended to achieve the best possible results.
Can Varicose Veins Return After Vein Glue Treatment?
Unfortunately yes, varicose veins can return even after you had a vein glue treatment, despite the treatment being really effective. It’s because vein glue treats the troubled veins at the moment, once the treatment is done these veins will close off, but the other existing veins can always develop into varicose veins, and since we can never know which veins will turn into varicose veins in future, their return is possible. There are more chances of this happening if you have varicose veins because of an underlying condition like genetics, lifestyle or poor blood circulation. That’s why you must make sure to follow preventive tips to reduce the risk of developing varicose veins after the treatment.
How Soon Can I Return To Normal Activities After The Treatment?
The good news is that, vein glue is a minimally invasive treatment which means you can return to your normal lifestyle right after the treatment! However, the only tip you need to follow is avoiding strenuous activity for one to two weeks as they can interfere with the procedure and recovery. Your will be recommended to wear compression stockings as well to support healing, which will speed up the healing as well.
What Follow Up Treatment Is Needed?
Here’s some follow-up treatment after vein glue:
- Compression Stockings: As mentioned earlier it helps with faster recovery!
- Physical Therapy: Light walking will be encouraged to promote blood circulation, but strenuous activities must be avoided at all costs.
- Monitoring: Go for all the follow-up appointments to check for any complications.
- Avoid Heat: Make sure to avoid hot baths, direct sun light, and saunas for few days.
Is Vein Glue Safe For Older Adults?
Yes, since it’s a minimally invasive treatment, it’s extremely safe for older adults!
How long does it typically take to see noticeable results after vein glue treatment?
Patients can often see noticeable results within a few weeks to a few months after vein glue treatment. Initially, there may be some bruising and swelling, but as the treated vein closes and the body absorbs it, the visible symptoms, such as bulging or discomfort, should improve. The exact timeline can vary depending on the individual’s healing process, the size of the treated vein, and the severity of the vein issue.

